CLINICAL MASS SPECTROMETRY SERVICES
DISCOVERY & TARGETED CLINICAL MS SERVICES
Service: VP-CLIN LC-MS/MS
HRMS/QQQ IN CLINICAL RESEARCH:TARGETED QUANTITATION TO METABOLOMICS
Clinical mass spectrometry uses the mass spectrometry technology for diagnostic purposes. Employed by medical labs, clinical mass spectrometry is used to diagnose metabolism deficiencies, to determine whether biomarkers or enzymes are present, and for toxicology testing.
Clinical diagnostic mass spectrometers can analyze a small amount of sample for many things at once, making them a valuable tool for a diagnostic medical laboratory. One of the new ways that clinical mass spectrometry is being used is to quantitatively detect small amounts of proteins, biomarkers, or drug molecules, even when their concentrations are low. The ability to use small samples with low concentrations has allowed researchers to determine pharmacokinetic profiles of drugs that have been given in microdoses. This protects the patient from possible adverse effects of the drug while allowing scientists to determine what happens to the drug in the body.

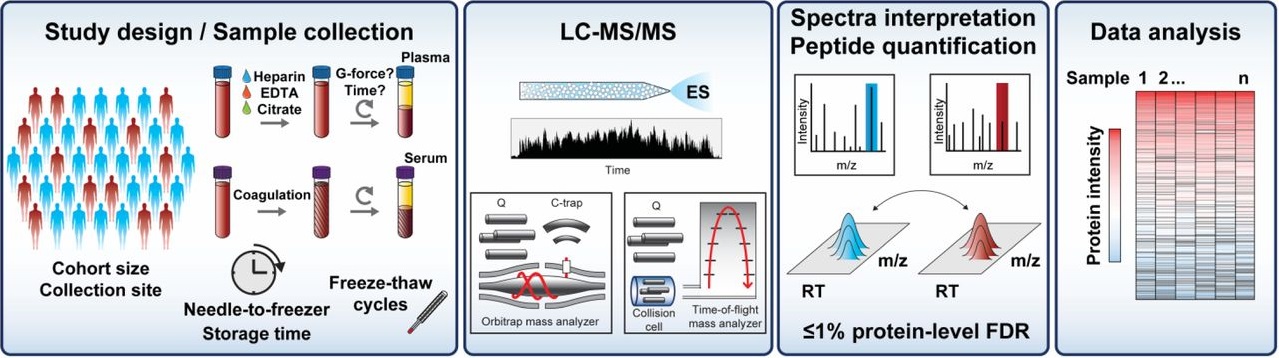
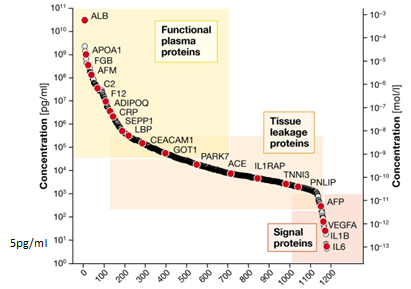
Plasma Proteomics:
BIOMARKER STUDIES
Vitamin D estimation
Vitamin-D and parathyroid hormone (PTH) are the principle regulators of calcium homeostasis in all tetrapods and play an important role in bone metabolism
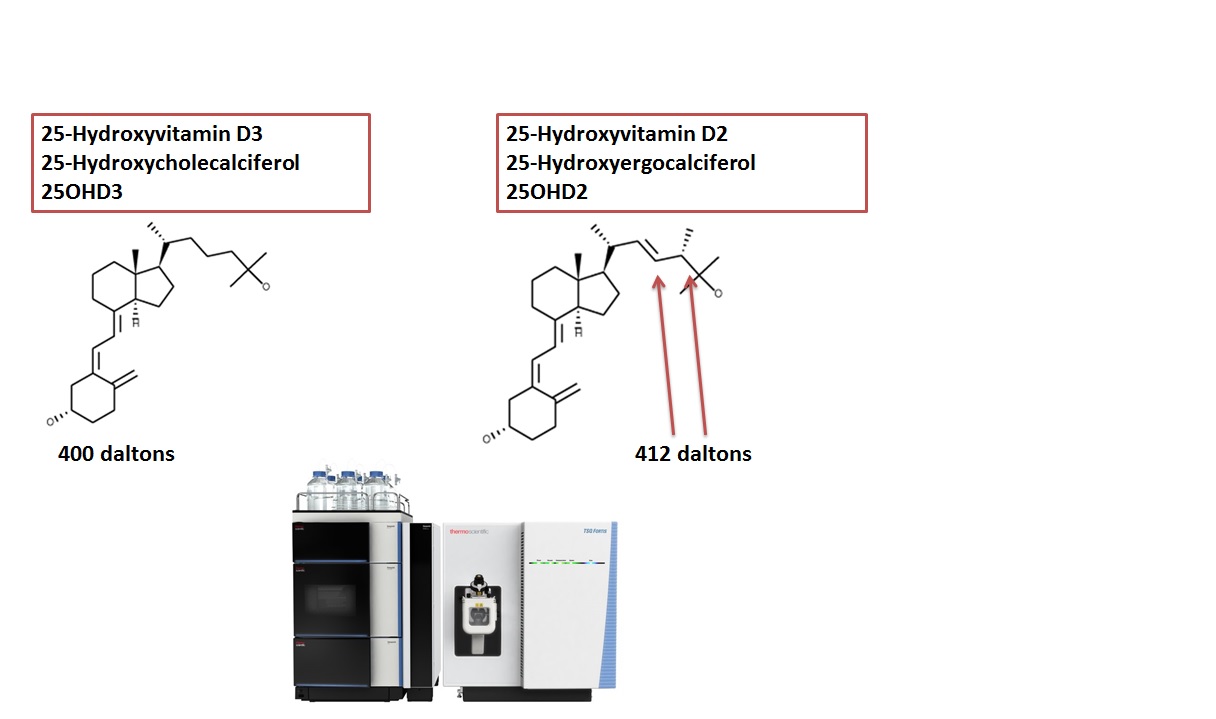
Vitamin-D exists in two major forms, vitamin-D2 (ergocalciferol) and vitamin-D3 (cholecalciferol). Both are formed by UV irradiation of either 7-dehydroergosterol (phytoplankton, fungi and yeast) or 7-dehydrocholesterol (all vertebrates with the exception of fish [predominately dietary-derived vitamin-D2]). The two forms differ only in the substitution on the side chain.
In modern humans, primary sources of vitamin-D include diet or supplements (vitamin-D2 and/or-D3) and vitamin-D3 derived from 7-dehydrocholesterol in the skin after exposure to UV light. Since vitamin-D3 and vitamin-D2 are either stored in adipose tissue or rapidly metabolized to the corresponding 25-hydroxylated metabolites, their serum levels fluctuate widely and there is no clinical value in monitoring these forms of vitamin-D in the circulation.
Among the >40 vitamin-D metabolites discovered so far, three have been shown to be the most clinically relevant: 25(OH)D, 1,25(OH)2D and 24,25(OH)2D.
Methodologies for 25(OH)D measurements include high performance liquid chromatography (HPLC), radioimmunoassay (RIA), automated immunoassays and liquid chromatography-tandem mass spectrometry (LC-MS/MS), while current 1,25(OH)2D and 24,25(OH)2D measurements involve RIAs or LC-MS/MS. Analytical challenges have been reported for all of these methods (Singh, 2008), but currently measurement of vitamin-D compounds by HPLC with MS/MS detection (Heijboer et al., 2012; Eisman and Deluca, 1978) has been established as the gold standard for vitamin-D metabolite testing
LC-MS/MS overcomes these analytical challenges and has become widely accepted for routine use for many low molecular weight analytes in clinical laboratories due to improved analytical specificity and sensitivity and wider dynamic range compared to immunoassay methods
What is the recommended level of vitamin D in Blood?
The recommended blood levels of vitamin D – is more than 30ng/ml
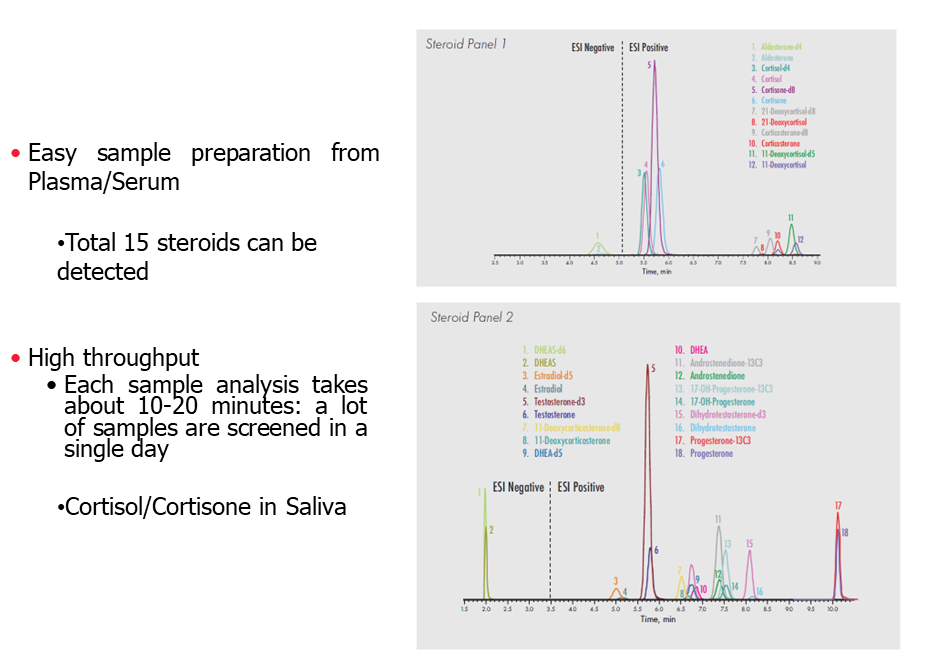
Steroid Panel Screening
Steroids are synthetic hormones that are used to treat various medical conditions. However, these drugs are also used illegally by athletes and bodybuilders to enhance their performance and gain muscle mass. The misuse of steroids can lead to serious health problems, including liver damage, kidney failure, and heart disease.
Biosynthesis of active steroid hormones occurs in gonads, adrenal glands and other tissues. All these are synthesized by the enzymatic modification of cholesterol. Comprehensive assessment of steroidogenic biosynthetic pathway is useful to screen both common & rare forms of Congenital Adrenal Hyperplasia and other syndromes of adrenal hyper / hypofunction. This kind of assessment facilitates evaluation of precursors / product ratios thereby increasing diagnostic discrimination of adrenal enzymatic disorders.
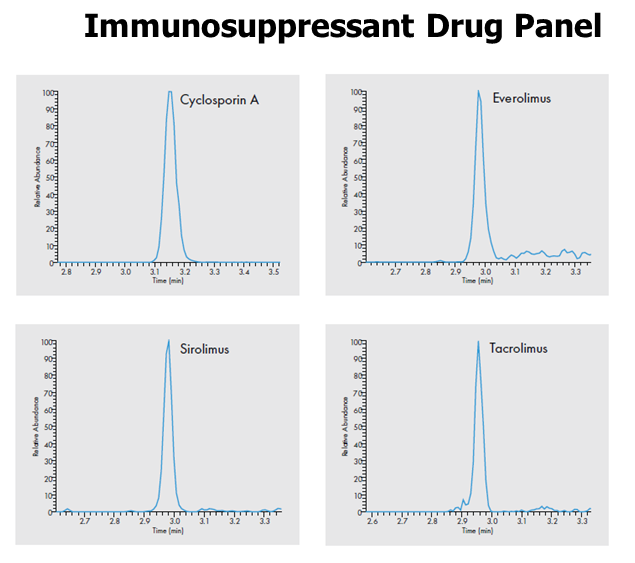
Therapeutic Drug Monitoring
Therapeutic drug monitoring is the measurement of specific drugs and/or their breakdown products (metabolites) at timed intervals to maintain a relatively constant concentration of the medication in the blood. Some of the monitored drugs tend to have a narrow “therapeutic index,” which is a ratio between the toxic and therapeutic (effective) dose of medication.
As soon as a drug enters the body, different processes start removing the drug from the body. The amount of time it takes for the body to reduce the drug concentration to half from the initial value is called a half-life of the drug. It generally takes around five half-lives to remove a drug completely from the body.
Generally, a person must be given a drug dose at regular intervals to ensure that the effective or the therapeutic concentration of the drug is maintained in the body. For some drugs, maintaining this steady state is not as simple as giving a standard dose of medication. Each person will absorb, metabolize, utilize and eliminate drugs at different rates based upon their age, general state of health and genetic makeup. The drug concentration in the body may be enhanced or decreased by the interference of other medications that you may be taking along with the drug which has to be motioned. This is also known as drug-drug interaction.
Not all medications require therapeutic monitoring. Most drugs have a wide therapeutic index and can be prescribed based upon pre-established dosing schedules. The effectiveness of these treatments has been evaluated, but monitoring the concentration of the drug in the blood is not required for dosing. Examples of drugs that do not require monitoring include high blood pressure (hypertension) medications and many of the antibiotics given to treat bacterial infections. If an infection resolves with a given antibiotic or if blood pressure is lowered with the prescribed blood pressure medication, then the treatments have been effective.